The Sangamon County Department of Public Health (SCDPH) is investigating a
single case of monkeypox virus infection (MPV) in an adult man who presented with
symptoms to a health care provider.
Initial testing was completed on July 26, 2022, at an Illinois Department of Public Health (IDPH) Laboratory. Confirmatory testing is pending at the U.S. Centers for Disease Control and Prevention (CDC).
Based on initial epidemiologic characteristics and the positive orthopoxvirus result at IDPH, health officials consider this a probable MPV infection. SCDPH and IDPH are working closely with the CDC, the patient, and the patient’s health care providers to identify individuals with whom the patient may have
been in contact while they were infectious.
This contact tracing approach is appropriate given the nature and transmission of the virus, and to coordinate timely risk assessment and appropriate post-exposure response. At this time, SCDPH has not identified any additional cases in the county.
The case remains isolated and at this time there is no indication there is a great
risk of extensive local spread of the virus, as monkeypox does not spread as easily as the COVID-19 virus.
Person to person transmission is possible through close physical
contact with body fluids, monkeypox sores, items that have been contaminated with
fluids or sores (clothing, bedding, etc.), or through respiratory droplets following
prolonged face-to-face contact.
Since May 14, 2022, clusters of monkeypox cases have been reported in several
countries that don’t normally have monkeypox. On May 20, 2022, the CDC issued a
Health Advisory regarding recent cases in the United States. As of July 26, 2022, the
CDC reports 3,591 confirmed cases of orthopox/monkeypox across 46 States, including Illinois.
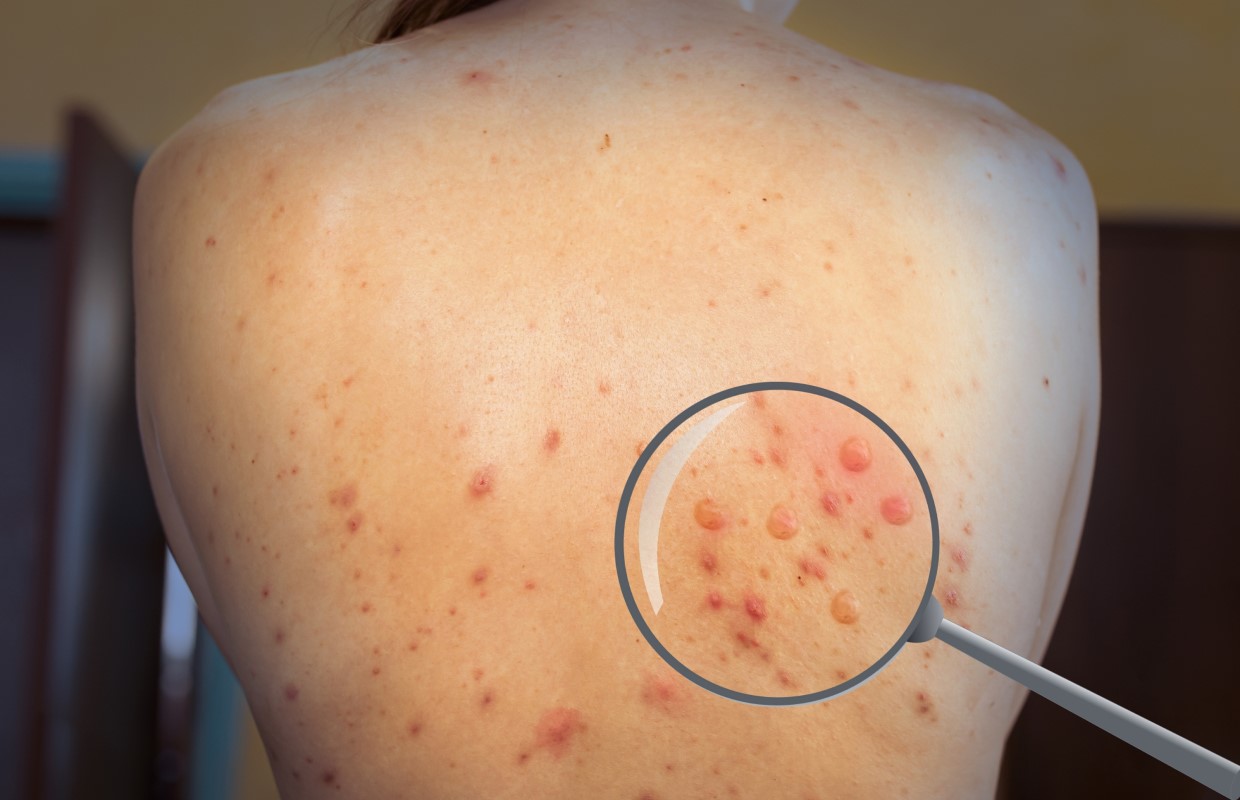
Monkeypox is a rare, but potentially serious viral illness, which belongs to the
Orthopoxvirus family, and typically begins with flu-like symptoms and swelling of the
lymph nodes, and progresses to a rash on the face and body. Most infections last 2 to 4 weeks.
Monkeypox is typically endemic to parts of central and west Africa, and people
can be exposed through bites or scratches from rodents and small mammals, preparing wild game, or having contact with an infected animal or possibly animal products.
It’s not clear how the people were exposed to monkeypox, but early data suggest
that gay, bisexual, and other men who have sex with men make up a high number of
cases. However, anyone who has been in close contact with someone who has
monkeypox is at risk.
Public health officials are urging healthcare providers in the U.S.
to be alert for patients who have rash illnesses consistent with MPV, regardless of
whether they have travel or specific risk factors for monkeypox and regardless of gender or sexual orientation.
Anyone with a rash that looks like MPV should talk to their healthcare
provider, even if they don’t think they had contact with someone who has monkeypox.
People who may be at higher risk might include but are not limited to those who:
1. Had contact with someone who had a rash that looks like monkeypox or someone
who was diagnosed with confirmed or probable monkeypox
2. Had skin-to-skin contact with someone in a social network experiencing
monkeypox activity, this includes men who have sex with men who meet partners
through an online website, digital application (“app”), or social event (e.g., a bar
or party)
3. Traveled outside the US to a country with confirmed cases of monkeypox or
where monkeypox activity has been ongoing
4. Had contact with a dead or live wild animal or exotic pet that exists only in Africa
or used a product derived from such animals (e.g., game meat, creams, lotions,
powders, etc.).
For more about this virus, visit www.cdc.gov/poxvirus/monkeypox